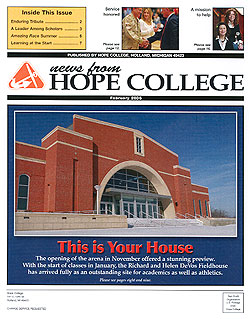
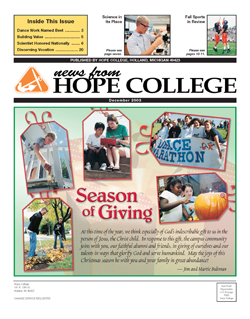
For This Medical Device, Paper May Be Just the Ticket
Kenneth Brown, Ph.D. | Professor of Chemistry
A pricked finger, a drop of blood, a glucose level readout.
The routine is familiar to anyone with Type 2 diabetes, and a team of researchers at Hope is working to shake it up. Not the prick to the finger, but to the wallet.
Over two months in mid-2019, Dr. Kenneth Brown noticed that the price of diabetes blood-glucose test strips tripled. He’s been working for three years to reverse that trend.
“Currently, the test strips are made out of plastic,” Brown says. “What we would like to do is look at using paper as a platform. That could significantly lower the cost of the test strips. Some companies charge as much as $2 per test strip” — and patients require two per day. Brown hopes to reduce the unit cost to 5 cents.
The platform — the structural material of the strip — is key. It is the track for a relay race of sorts that brings glucose data from a drop of blood into a monitor to generate a legible readout.
Blood carries all sorts of nutrients, including glucose, around the body. Some individuals with diabetes don’t produce enough insulin to take that glucose out of the bloodstream and into their cells, where it can be used immediately for energy or stored for later use; for others, the problem is insulin resistance, which occurs when cells in muscles and fat don’t respond well to insulin. Consequently, people who have diabetes must monitor their blood-glucose level and inject insulin — or take oral medication — to compensate.
Monitoring is a seven-second process that starts with insertion of a testing strip into a glucose meter. Next come a finger prick and application of a drop of blood to the testing strip. Glucose in the blood reacts with an enzyme that during the manufacturing process was applied to the strip’s polymer-coated platform; the enzyme triggers the oxidation of glucose, which releases electrons. The displaced electrons are transferred through the polymer coating to the strip’s end and “read” by the meter’s electrodes. The device displays the glucose level in numeric form.
“The significant breakthrough is that we can make our polymer coatings onto a paper-based platform,” Brown says. “The compound we’re using is not commercially available, so we synthesize a carbon paste in our lab and that is applied to the paper. We then use electrochemical techniques to form polymer coatings on paper via the carbon paste.”
Other scientists are working on different innovations, including a device that attaches to one’s arm or shoulder and continuously monitors one’s blood-glucose level, sending updates directly to a smartphone. The drawback is that such devices work for a period of perhaps 10 days before the entire machine needs to be replaced—at a cost of about $100, substantially more than 10 days’ worth of test strips. “I do believe that the work that we are doing could have a very significant impact upon those who are in a place where these test strips are a medical necessity,” Brown says.
For 12 years, since receiving his diagnosis of Type 2 diabetes, Brown has been one of those. His research may have saved his life; it certainly contributed to his diagnosis. “What really prompted me to go to the doctor was that my students noticed what was going on,” he shares. Brown’s energy level was getting unpredictable; his clothes were getting baggier. His students connected the dots.
“My research would not be possible without my students,” he says. “I don’t think of my students as working for me, but rather they’re working alongside me.” That partnership has resulted in a functioning prototype of a paper-based test strip, whose durability and functionality Brown and his student research assistants hope to improve. He envisions a strip that could someday be used for more than one glucose reading, and for an even more accurate reading.
Each test strip packs an impressive amount of technology for a tiny, single-use object. “When you think about all the different chemicals that are in the body, being able to detect glucose in the presence of all these other molecules is a very challenging problem,” he says. “One of the goals is to make this process easier.”
Brown’s project began with the polymer coating — the material on the test strip that allows for the detection and measurement of glucose in a drop of blood. The project evolved to tackle improving the detection capability of the coating, create a paper based platform for it, and increase the durability of that platform.
Brown has a favorite quote, familiar in Reformed circles: “Where your talents and the needs of the world cross, there lies your vocation.”
“When I read this, I think about the cross of Christ,” he says, “because the cross of Christ is an intersection between humanity and God. I think about the gifts that God has given us; one of those gifts is knowledge. Every day, we are learning more and more about the human body. That tells me about the infinite God we serve.” Serving God through teaching and learning, working alongside student researchers, is a calling and a mission — one that Brown intends to have outlive him.
“My motto is: ‘Success without a successor is failure,’” Brown says. “And for me, that’s part of a faith dimension. Seeing my students go out and do much more than what I’ve done — seeing them impact the world for good — speaks volumes of what Hope instills within students.”